If you’re wondering how can you treat psoriasis at home?, you’re seeking a practical and proactive approach to managing a chronic skin condition. While true healing may require professional care, many supportive measures can significantly ease symptoms, reduce flare-ups and help you feel more in control. This detailed guide will walk you through proven home-based strategies—covering skin care, diet, lifestyle, and when to seek medical intervention—that align with the same user-friendly, SEO-optimized style you’re familiar with.
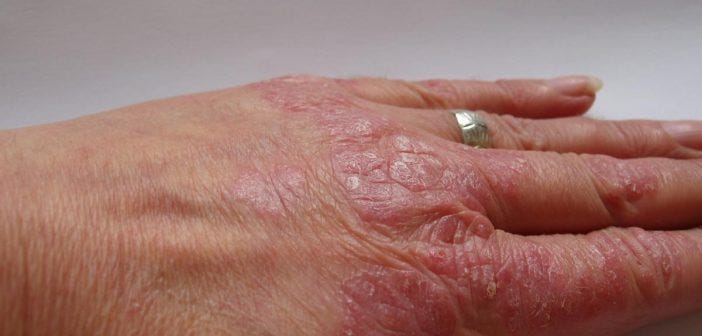
How Can You Treat Psoriasis at Home? – A Comprehensive Guide
1. Understanding Psoriasis & Why Home Care Matters
Psoriasis is an autoimmune-linked skin condition characterised by rapid skin cell growth, causing red, scaly patches (plaques) that can itch, hurt or crack.
Although a full “cure” may not be feasible for everyone, home care plays a vital role in:
- Reducing symptom severity and frequency of flare-ups
- Supporting standard treatments prescribed by your dermatologist
- Improving comfort, appearance and overall skin health
- Reducing triggers like dryness, stress or lifestyle factors
Important note: Home-remedies are for support—they’re not a substitute for medical advice or prescription treatments when needed.
2. Skin-Care & Bathing Habits for Psoriasis Relief
A) Gentle Cleansing & Moisturising
- Use lukewarm water (not hot) and mild, fragrance-free cleansers. Hot water may worsen dryness or trigger plaques.
- Immediately after bathing, while skin is still slightly damp, apply a rich ointment-based or heavy cream moisturizer to lock in moisture.
- Use a humidifier in dry climates/rooms to keep indoor air moist and support skin barrier.
B) Soaks & Baths That Support Relief
- Colloidal oatmeal baths or Epsom/Dead Sea salt baths help ease scaling, itching and dryness. A 15-minute soak in lukewarm water with these additives may soothe skin.
- After a soak, moisturise right away to seal in hydration.
C) Targeted Treatments
- Apply 0.5% aloe vera gel or creams (or plant-based equivalents) regularly on affected patches; some evidence supports its use.
- Salicylic acid or tar-based cleansers/ointments may help loosen scale and reduce plaque thickness—but should be used carefully and preferably under guidance.
- Always protect skin from scratching or trauma; injuries can trigger new plaques due to the Koebner phenomenon.
3. Daily Lifestyle & Diet Support for Psoriasis
A) Anti-inflammatory Diet
Since psoriasis involves immune-inflammation, dietary support helps:
- Increase: oily fish (omega-3s), leafy greens, colourful vegetables, nuts and seeds. These help regulate inflammation.
- Limit: processed meats, high sugar, saturated fats—these may exacerbate psoriasis.
- Consider vitamin D, curcumin (turmeric) or fish-oil supplements (after discussing with your healthcare provider) as supportive strategies.
B) Managing Weight, Stress & Sleep
- Excess body weight correlates with more severe psoriasis; thoughtful weight management helps.
- Stress and poor sleep can trigger or worsen flare-ups—incorporate relaxation techniques (meditation, yoga, deep-breathing) and aim for restful sleep.
C) Controlled Sunlight & Exposure
- A moderate amount of sunlight (UVB) may improve psoriasis in some people—but avoid sunburn, tanning beds or excessive exposure which can backfire.
- Always apply broad-spectrum SPF on unaffected skin and protect it properly.
4. Identifying and Avoiding Triggers
- Keep a journal to track what may trigger your flare-ups: infections, alcohol, smoking, stress, medications or skin trauma.
- Avoid scratching, harsh fabrics, tight clothing or exposures that irritate your skin.
- Quit or reduce smoking; studies indicate smoking worsens psoriasis.
5. When to Seek Medical Help
You should consult a dermatologist if one or more of these apply:
- Widespread plaques covering large areas or ears, scalp, palms/soles
- Signs of skin infection (pus, warming, pain)
- Joint pain or swelling suggesting psoriatic arthritis
- Intense flare-up unresponsive to home measures
- Sudden onset after new medication or major illness
Even when using home-care strategies, your specialist will guide safe combinations with topical or systemic treatments.
6. What to Expect: Timeline, Realistic Outcomes & Consistency
- Short-term (2–4 weeks): With consistent bathing, moisturising and diet/lifestyle changes, you may see less redness, softer scaling and fewer itch episodes.
- Mid-term (3–6 months): Flare-ups may become less frequent or severe; you might find you can maintain skin more stable with fewer interventions.
- Long-term: Psoriasis is often a chronic condition. The aim is regular control and good quality of life rather than “perfect” skin. Home-care routines build resilience and reduce impact.
7. Mistakes & What to Avoid
- Relying only on home remedies and ignoring professional advice when needed.
- Over-exposure to sunlight, tanning beds or hot baths believing “more = better”—which can worsen psoriasis or raise skin-cancer risk.
- Using harsh exfoliants/scrubs that aggravate sensitive plaques.
- Dismissing the role of skin barrier repair and moisturising.
- Jumping between many “quick fix” remedies without consistent routine—consistency matters more than novelty.
Final Thoughts
Treating psoriasis at home is absolutely possible—when done thoughtfully, consistently and in harmony with your healthcare support. By focusing on gentle skin care, hydration and moisturising, diet and lifestyle alignment, trigger awareness, and when necessary medical intervention, you give your skin the best environment to heal, calm and maintain. Remember: each person’s journey is different—what works for one may need adjustment for you. Patience, self-care and smart habits pay off.